Venous insufficiency occurs when leg veins stop working efficiently. An estimated 40 percent of people in the United States have venous insufficiency, or CVI (“chronic venous insufficiency”).
What is Venous Insufficiency?
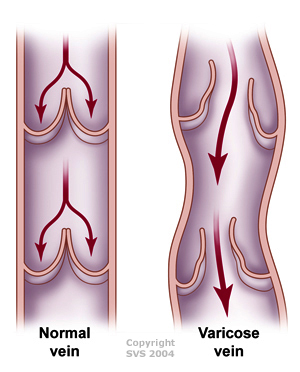
The function of veins is to bring blood back to the heart. Because leg veins work against gravity, they contain one-way valves that prevent the blood from flowing backward as it travels back to the heart.
If a valve becomes weak, blood can leak back down and become pressurized in the veins. This causes what is known as venous insufficiency, vein reflux, or venous reflux. Veins will then start to bulge out on the legs, creating the condition known as varicose veins.
Since there is both a deep and superficial venous system in the legs, venous insufficiency can be superficial, deep, or a combination of both.
Causes of Venous Insufficiency
In many cases, venous insufficiency is caused by genetics. If you have a family history of venous insufficiency or varicose veins, you are more likely to develop them as well.
Other factors that can cause venous insufficiency include:
- Age
- Obesity
- Smoking
- Pregnancy
- Prolonged periods of sitting/standing
- Leg injury or surgery
On average, venous insufficiency occurs more frequently in people over the age of 50, and more often in women than in men.
Symptoms of Venous Insufficiency
Venous insufficiency may not cause any immediate pain, but there are several other symptoms to look for:

- Leg / ankle swelling
- Itching
- Aching
- Throbbing
- Heaviness
- Varicose veins
- Leg cramps or muscle spasms
- Tightness in calves
- Restless leg syndrome
- Pain when walking
- Thickening of skin
- Brown ankle skin
- Leg ulcers
The symptoms of chronic venous insufficiency may seem like other health conditions. Meet with a vein specialist for a diagnosis.
Diagnosis & Treatment for Venous Insufficiency
A healthcare provider will take your medical history and provide an exam, which may include an ultrasound. This evaluates the blood flow and structure of your leg veins.
Once a patient is found to have venous insufficiency, proper treatment will depend on their current symptoms. This may include:
Compression Stockings
These elastic socks apply pressure to the legs and help blood flow more efficiently. Compression stockings come in various lengths, pressures, and styles, so a vein specialist should help find the perfect fit.
Leg Elevation
Keeping legs elevated during rest can reduce swelling and improve blood flow.
Exercise & Movement
Avoid sitting or standing for long periods of time. If you have to sit for a long while, stretch or flex your feet, ankles, and legs often. Take breaks from standing to rest.
Any exercise, especially walking, is a great way to help strengthen legs and keep blood flowing.
Medications
In the event of leg ulcers, medicines that increase blood flow may be used alongside other methods to help them heal. Antibiotics or aspirin may be recommended.
For patients who have and/or are prone to blood clots, anticoagulants may also be prescribed.
Non-Surgical Procedures
If venous insufficiency has developed enough, a minimally-invasive procedure may be necessary to reduce symptoms. Depending on your condition, a vein specialist may recommend radiofrequency ablation (RFA) like Closurefast, a medical adhesive like VenaSeal, or sclerotherapy like Varithena.
Vein Surgery
Less than 5% of patients need surgery for venous insufficiency. In severe cases, options will include ambulatory phlebectomy, vein stripping/ligation, vein valve transplant, and others.
Would You Like to be Evaluated for Venous Insufficiency?
Fill out our Online Vein Screening Form to set up a consultation or call any of our clinics in Northwest Portland , Tigard, Happy Valley, Hillsboro or Bend, Oregon.