When the valves in our leg veins become weak, either from heredity or injury, blood can pool in the lower legs under pressure. This leads not only to swelling, but also to skin damage. With time the skin can break open, known as a venous stasis ulcer. Also known as a venous leg ulcer, these are chronic wounds on the lower leg – typically around the ankle. One characteristic is that they can be very slow to heal or not heal at all without treatment.
Leg ulcers sometimes spontaneously open up, or develop after a minor injury. This is a progressive problem and there are causes & conditions that can lead to venous ulcers.
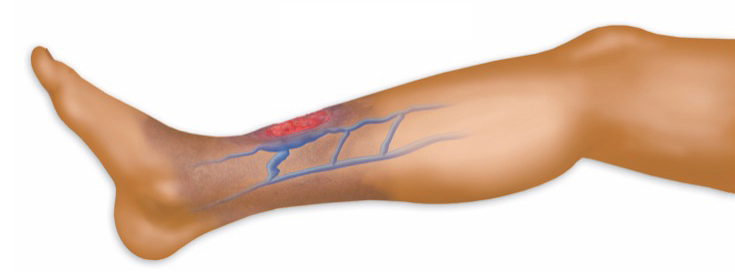
The primary underlying cause is chronic venous insufficiency. If the underlying cause of the ulcer is not treated, venous ulcers will fail to heal or repetitively return.
Symptoms of Venous Ulcers
Patients who experience venous ulcers often have long-standing venous insufficiency and experience high venous blood pressure in the lower legs for an extended period of time. This can occur even when varicose veins are not visible on the surface of the leg.
Venous leg ulcers are often associated with:
- Swollen ankles
- Skin discoloration around the ulcer
- Hardened skin around the ulcer
- Heaviness in the legs
- Aching in the legs
- Varicose eczema
- Varicose veins
Signs of an Ulcer Infection
Because they are open wounds, a venous leg ulcer can be prone to bacterial infection.
An ulcer may be infected if patients experience:
- Pain that gets worse
- Discharge that can be green or foul-smelling
- Redness and swelling around the ulcer
- Fever if there is surrounding infection
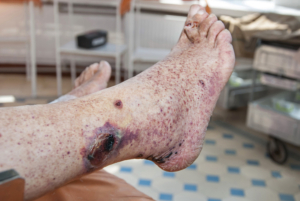
Many venous ulcers look infected, even though most are not. Most are colonized with bacteria but that does not mean there is an invasive infection in the tissue around them.
However, for those that do become infected, this infection can be life-threatening and may require hospitalization and/or long-term IV antibiotics. The surrounding infection is known as cellulitis or lymphangitis. This is why it’s important for all venous ulcers to be evaluated as early as possible by a vein or vascular specialist since early treatment can reduce the risk of infection leading to hospitalization.
Call 1-800-834-6362 to Schedule a Consultation or Use Our
Frustrations Around Non-Healing Leg Wounds
There are other types of non-healing leg wounds, but venous ulcers are a highly common cause.
When a patient visits one of our offices with a venous stasis ulcer, they are often frustrated with a wound that has been on going and has not yet healed. Some have had the venous ulcer for many years, as their small wound has opened up, become larger, and failed to heal. We often hear:
- Patients have seen multiple doctors and clinics, without any luck in figuring out what is wrong.
- Patients may not have been told by other providers that their non-healing leg wound could, in fact, be due to venous insufficiency.
- Patients often think they had a bug bite, or assume the wound is entirely due to an infection.
At Inovia Vein Specialty Centers, we specialize in Venous Stasis Ulcer Treatment and we have the diagnostic tools and experience needed to help make an accurate diagnosis and develop a definitive short-term and long-term treatment plan. We can both diagnose and treat these problems in our office without having to send patients out for more tests.
Why Choose Inovia Vein Specialty Centers
Most vein specialists perform treatments in hospital settings, where higher costs and added barriers can make care more complicated and less accessible. Inovia Vein Specialty Centers is entirely office-based, allowing us to provide high-quality, specialized vein care in a comfortable, convenient environment, while keeping treatment more affordable and easier to access. Originally founded in Bend, Oregon, Inovia Vein has grown across Oregon and into Southwest Washington, becoming the Pacific Northwest’s largest vein-centric healthcare practice.

At Inovia Vein Specialty Centers, you’ll find patient-centered care from some of the region’s leading, board-certified vein specialists. We partner with you from consultation through treatment and follow-up, offering comprehensive diagnostics and advanced, minimally invasive therapies designed to heal venous leg ulcers and help prevent recurrence. By combining trusted expertise with state-of-the-art technology and a commitment to innovation, our team delivers safe, effective solutions in convenient locations.
Frequently Asked Questions
Venous Leg Ulcers
Studies have shown that the sooner one sees a vascular or vein specialist and the sooner the patient is treated, when indicated, with endovenous ablation, the faster the wound heals. Therefore, while wound care is important in the initial management, so is referral for consideration for superficial vein ablation.
Most venous leg ulcers will heal with consistent and adequate control of the swelling, proper wound care and endovenous ablation of the varicose veins contributing to the ulcer. Some however, do not heal, and may have other contributing factors beyond just the vein issue. Dermatologic disorders, cancer in the wound, and other risk factors such as obesity, heart failure, and/or lack of mobility from severe back or orthopedic issues can all contribute to a wound’s ability to heal. If you have had prior vein treatments and venous leg ulcers have returned, its advisable to seek further medical attention for a biopsy, when indicated, and to discuss ongoing management options. If you have had treatment and the wounds does not heal, you should discuss this with your providers to look at other potential contributing factors that are preventing healing.
The sooner the better. Unfortunately, many patients have had ulcers for years and have never been referred or found a vascular specialist. We keep appointments open for short notice add-ons for patients with new or long-standing venous leg ulcers, so they can get in and start the process to healing as soon as possible. We can at least start the process, so the proper treatment comes sooner rather than later.
Yes. Studies have shown that the sooner a patient with a venous leg ulcer is referred to a vascular specialists, the sooner the ulcer can be treated so it will heal faster. At Inovia Vein Specialty Centers, we encourage early referral so our vascular specialists can start the process to get patients into endovenous ablation, when indicated, sooner rather than later.
Nearly all are the same thing. However, a vascular ulcer could be from arterial or venous . Arterial ulcers are different than venous ulcers. An arterial ulcer tends to be on the toes or bottom of the foot whereas the venous ulcers tend to be on the lower ankle, back of the calf or sides of the foot. A venous or vascular expert can usually help sort this out so the most optimal treatment is utilized to get the ulcer healed.
Treating a venous leg ulcer entirely at home is not recommended. Most patients with venous leg ulcers are managed as outpatients; they see vein and vascular specialists in the office setting and a wound care plan is developed then implemented. From there, the goal is to allow the patient to manage their wounds at home. Sometimes, especially at first, there are many visits for wound dressing changes and vascular studies. These procedures can be completed in either the outpatient or hospital setting. The outpatient setting is far more convenient and less cost than the hospital. Rarely, if a patient has a severely infected wound, hospitalization is required.
It depends on how wet they are. Wet wounds generally need to be covered, where as dry scabbed over wounds do not. A dry wound that is scabbed over has natural protection and may even do well in a compression stocking. But if there is any wetness, it will cause the dressing or stocking to stick, which will injure the healing skin when the dressing comes off. Thus a wet wound needs a wound care regimen that will not stick to the wound. One of the most reliable approaches to a wet, painful venous leg ulcer is an Unna Boot, which is a special medicated soft dressing that does not stick to wounds and can be applied with pressure to help treat the swelling as well. There are many ways to treat a wound an most wound experts have many resources at their disposal to help.
Chronic venous insufficiency with high vein pressure creates a highly inflammatory environment where wound healing is impaired. Treating the cause - venous hypertension, is the mainstay of treatment of venous leg ulcers – along with adequate wound care and compression are all important for treatment.
Venous leg ulcers usually start out in the area by the inner upper ankle, back of the lower calf, or lateral or medial foot. The skin there has usually been red, hard or brown for some time. A wound opens and it is painful in most cases. Then it fails to heal. They can be small or quite large.
Ideally, venous leg ulcers can be prevented with compression hose and, when indicated, with endovenous ablation of the superficial veins where ulcers occur. However, most patients don’t see it coming, so the first time they present for care is once an ulcer opens up and won’t heal.
Those who have had chronic venous insufficiency, varicose veins, or deep vein thrombosis (DVT) are at the highest risk. Older adults, individuals who are overweight, smokers, and those who sit or stand for long periods are also more likely to develop venous leg ulcers.
Compression improves blood flow by helping veins push blood back toward the heart. This reduces swelling, lowers venous pressure, and creates an environment that supports wound healing.
Healing time depends on the size of the ulcer and overall health. With proper treatment, many ulcers improve within weeks and may fully heal within three to four months. Larger or long-standing ulcers may take longer to heal.
Poor circulation, uncontrolled swelling, infection, smoking, diabetes, obesity, and inconsistent use of compression can delay healing. Failing to treat the underlying vein condition can also prolong recovery
They rarely heal completely without treatment. Even if they temporarily close, they often reopen unless the underlying venous insufficiency is properly managed.
Dressing changes depend on the wound’s size, drainage, and type of dressing used. Some may need daily changes, while others can be changed every few days.
Antibiotics are only needed if there are signs of infection, such as increased redness, warmth, pus, fever, or worsening pain. Not all venous ulcers require antibiotics.
Avoid prolonged standing or sitting without movement, skipping compression therapy, smoking, and neglecting wound care instructions. Do not use over-the-counter creams or remedies without medical guidance.
Protein, vitamin C, zinc, and iron, along with adequate calories, supports tissue repair. Staying hydrated and managing blood sugar levels are also important for healing.
Wearing compression stockings as recommended, staying active, elevating your legs, maintaining a healthy weight, and treating underlying vein disease can significantly reduce the risk of recurrence.
Discover Lasting Relief with Venous Leg Ulcer Care in Portland, OR
Venous leg ulcers don’t have to control your comfort or quality of life. With expert evaluation and advanced, office-based vein care, lasting healing is possible. Call 1-800-834-6362 today to schedule your appointment and take the first step toward healthier legs and long-term relief.