At the Inovia Vein Specialty Centers, our focus is exclusively on the treatment of varicose veins.
At our specialty vein centers in Oregon, varicose veins are one of the most frequently treated issues we address for our patients. Varicose veins are swollen bulging veins under the surface of the skin that can be dark purple or blue in color. Although varicose veins can occur anywhere in the legs, they most often occur in the calves and behind the knees. Varicose veins develop on legs due to long standing venous insufficiency. Venous insufficiency leads to venous stasis, or pooling of blood in the lower legs, which can stretch out the veins leading to pain, swelling, and ultimately skin problems such as stasis dermatitis or venous stasis ulcers.
Venous insufficiency simply means some of the leg veins are not working efficiently enough. The function of veins is to bring blood back to the heart. Because the veins of the legs work against gravity, they contain one-way valves to prevent the blood from flowing backward as it travels back to the heart. If the one-way valve becomes weak, some of the blood can leak back down the vein, causing the veins to become pressurized in the veins. This causes what is known as venous insufficiency, vein reflux, or venous reflux. With venous reflux, veins start to bulge out on the legs. There is both a deep and superficial venous system in the legs. Venous insufficiency can be superficial, deep, or a combination of both.
Varicose Veins Causes
Venous reflux is a condition that develops when the valves that usually keep blood flowing out of your legs become damaged or diseased. When this occurs in the superficial veins, the congestion will cause the veins to abnormally enlarge, which in turn leads to either varicose veins and/or spider veins. When this happens over the long term, complications such as thrombophlebitis, deep vein thrombosis, chronic venous stasis changes in the skin and venous stasis ulcers can occur. The cause can be primary, for example from genetic influences, or secondary, due to damage to the vein valves from prior blood clots (Deep venous thrombosis) or phlebitis (superficial vein inflammation).
Varicose Veins Symptoms
While many varicose veins are asymptomatic, patients with bulging veins often complain that their legs feel heavy, or ache, and often their legs throb or feel more uncomfortable as the day goes on. Typically, these symptoms are worse at the end of the day and with prolonged standing. It is thought that these symptoms are due to a stretching of the veins as the blood abnormally pools in the leg vessels when the patient is standing. With time the skin by the ankle can become red, purple or brown, and inflamed whereby the patients complain of itching or burning of the skin. In some cases the inflammation is so profound over time the skin breaks down, leading to a venous stasis ulcer.
Expert Diagnostics
For many patients, an office evaluation by a vein specialist is all that is needed to determine the extent of the varicose and spider veins. At our Oregon vein centers in NW Portland, Tigard and Bend, this is the first step in developing an initial treatment plan.
In other patients, however, there is evidence that some of the larger superficial veins might be incompetent and contribute to the visible varicose veins. When this is suspected, a detailed examination using a sophisticated Duplex Doppler ultrasound scanner is done to ‘map’ the points of venous insufficiency and characterize the size and location of vessels.
This non-invasive test, performed in the office setting, allows the treating physician to better characterize the extent of the problem and develop a treatment plan that will minimize the chance of recurrence and maximize the potential to obtain the best results.
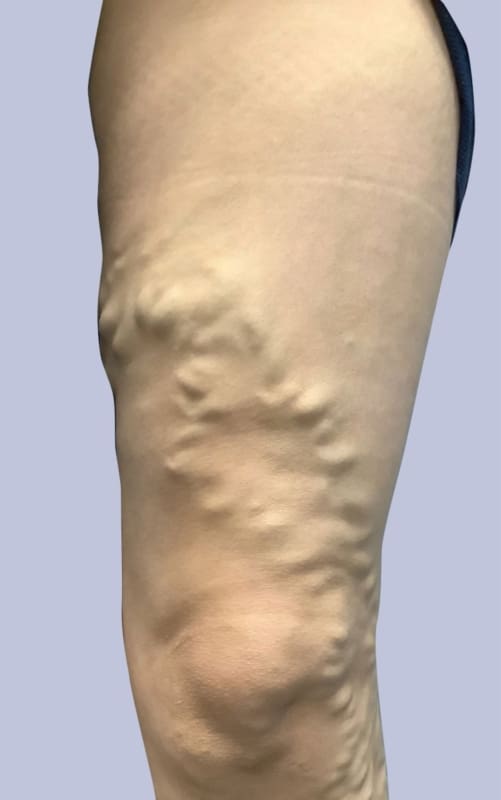
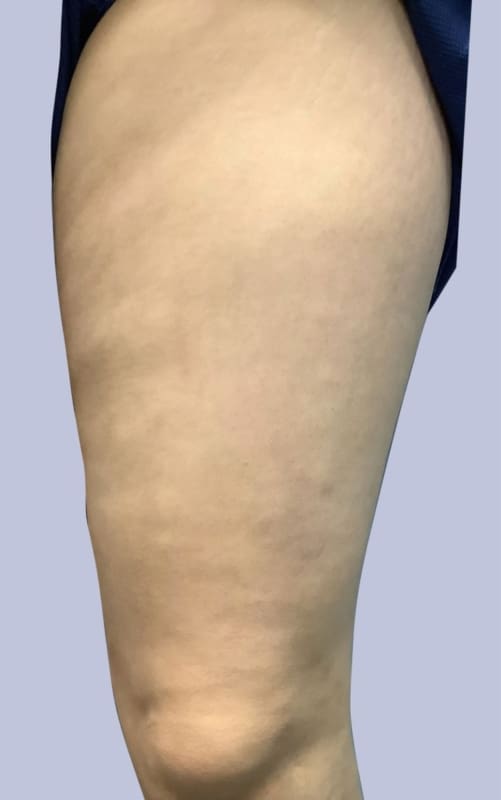
Used With Permission | Results May Vary
Ultrasound is also used after treatments to monitor progress, rule out complications, and assure optimal results. All this is performed on site in our vascular laboratory.
THESE PHOTOS ARE OF AN ACTUAL PATIENT OF OUR PRACTICE WHO HAS PROVIDED CONSENT TO DISPLAY THEIR PICTURES ONLINE. KEEP IN MIND THAT EACH PATIENT IS UNIQUE AND RESULTS MAY NOT OCCUR FOR ALL PATIENTS. PLEASE BOOK A CONSULTATION FOR MORE INFO ON HOW TREATMENTS MAY HELP YOU.
Treatment Options For Varicose Veins
There are a number of treatment options for patients with varicose veins. The most important first step is for the patient and care provider to consider the goals of the treatment. In many cases the goals are medical, when patients are seeking to reduce the symptoms of ache, swelling, heaviness, tiredness, night time cramping or skin issues such as stasis dermatitis or venous ulceration. In other cases the goal is cosmetic, when the patient is bothered by the appearance of of veins but not by these venous symptoms.
When the concern is cosmetic only on can begin procures promptly. For patients with larger bulging veins, an evaluation is done with an ultrasound, then a treatment plan is developed that may include Closurefast or Venaseal. When the issue is mostly reticular and spider veins, a plan can be developed for sclerotherapy.
However, when the goal is primarily a reduction in the symptoms of ache, swelling, heaviness, tiredness, night time cramping or skin issues such as stasis dermatitis or venous ulceration, we often begin with a conservative approach. This includes trying a program of exercise, elevation, and compression hose. The goal is to see if by undertaking these conservative approaches, the symptoms can be reduced. This program can be from 6 weeks to 3 months, and is often required by the insurance carriers. For patients who try but do not get adequate relief with conservative measures alone, a treatment plan can be developed to treat the veins with techniques such as Closurefast, Venaseal or Varithena. There are often subsequent sessions of sclerotherapy needed in many cases.
The goal is to minimize the degree of symptoms by treating these veins. Generally these procedures can result in considerable improvement in symptoms and a high degree of patient satisfaction. All of these procedures are done in our office. Patients come in, have their procedures, and go home, often in less than an hour. Downtime is minimal and many patients can go back to work the next day if they wish.
Call 1-800-834-6362 to Schedule a Consultation or Use Our
Are these treatments covered by insurance?
This depends on your policy and specific coverage provided by your insurance carrier. In general, most insurance providers divide vein treatments into one of two categories:
- Medically Necessary Procedures
- Cosmetic Procedures
Some vein treatments will fall under the category of cosmetic procedure, and as such, will not be covered by most insurance providers. This is commonly the case for asymptomatic spider veins. Another example is a patient with bulging varicose veins that do not ache, or bother them, but they seek treatment because of their concern about how the veins look cosmetically.
In this circumstance, however, insurance companies may deem varicose veins and other disorders medically necessary and thus will offer varying degrees of coverage depending on their contracts with the patient and the doctor. Insurance companies use varying criteria in order to determine if vein treatment is to be considered “medically necessary.” These criteria may include one or more of the following:
- Lifestyle Disruption: The daily activities of the patient must be disrupted significantly.
- Pain: The patient must be experiencing pain as a result of their vein disorder.
- Failure of Conservative Measures: Other methods of treatment, such as compression hose, have failed to provide adequate relief.
- Vein Size: Bulging veins larger than 4 mm are often considered medically significant.
- Complications: Complications, such as stasis dermatitis, phlebitis, bleeding veins, leg swelling and leg ulceration make it more likely an insurance company will consider treatment medically necessary.
A trial of conservative management is often required by the insurance carrier prior to providing insurance coverage for varicose vein treatments. This includes a number of features, such as compression therapy, rest, exercise, elevation and other maneuvers. If conservative therapy is beneficial in reducing the symptoms or complications of long standing varicose veins, then vein procedures such as endovenous ablation may not be needed. It is best to check with your insurance carrier if you have any questions about your coverage. We are also aware of these requirements and can help patients sort this out in many cases.
Recovery from Varicose Vein Treatment

Recovery from varicose vein treatment is typically quick and straightforward, thanks to minimally invasive techniques. Most procedures take place in the office with little to no downtime. Patients can usually return to daily activities the same day but should refrain from strenuous exercise and prolonged standing.
Mild bruising, swelling, or tenderness in the treated area is normal and usually resolves within a few days to weeks. Wearing compression stockings and regular walking can improve circulation, reduce discomfort, and promote healing. Follow-up appointments ensure optimal results and help prevent recurrence. While most patients experience significant symptom relief, maintaining vein health through lifestyle changes can support long-term outcomes.
Why Choose Inovia Vein Specialty Centers
At Inovia Vein Specialty Centers, we understand that vein problems in the legs are common, affecting over 30% of the population. Our mission is to provide high-quality, minimally invasive vein care in an accessible outpatient setting. Unlike many vein specialists who perform treatments in hospital environments—where costs and barriers are higher—we offer office-based procedures that make care more affordable and convenient. Our expert team helps patients find relief from varicose veins and other venous conditions with advanced diagnostic tools and state-of-the-art treatments while improving overall vascular health.
Founded in 2006 by Dr. Edward Boyle in Bend, Oregon, Inovia Vein Specialty Centers has become the largest vein-focused healthcare practice in the Pacific Northwest. Our expansion across Oregon and Southwest Washington reflects our commitment to making exceptional vein care available to more communities. Our board-certified specialists are leaders in the field, having participated in pivotal clinical trials and trained physicians internationally in cutting-edge vein treatment techniques. At Inovia Vein, we prioritize patient comfort, safety, and long-term results, ensuring that every patient receives the highest standard of personalized vein care.
Frequently Asked Questions
Varicose Veins
Treatments are usually minimally invasive, causing little discomfort. Patients may feel mild stinging or pressure during procedures, but local anesthesia enhances comfort. Recovery is generally quick, with minimal pain.
You should see a doctor if you experience pain, swelling, skin changes, non-healing sores, or varicose veins that interfere with daily activities.
Regular exercise, being at a healthy weight, keeping the legs elevated, avoiding lengthy sitting or standing, and wearing compression stockings can promote circulation and minimize vein pressure, helping to prevent progression.
Varicose veins can cause more serious complications like chronic swelling, skin ulcers, blood clots (deep vein thrombosis), and venous eczema. In severe cases, skin discoloration and painful sores may develop, impacting mobility and quality of life.
Early signs include leg swelling, aching, heaviness, itching, and cramping, especially after prolonged standing or sitting. Skin changes, such as discoloration or mild swelling around the ankles, can also indicate poor circulation before varicose veins become visible.
Patients are typically able to resume normal activities 24-hours after vein treatment, but travel may pose additional risks. Sitting in a car or airplane for several hours can increase the risk of a blood clot, so it’s important to know blood clot symptoms and understand ways to mitigate the risks. If a patient is planning a long trip, especially out of the country, we recommend rescheduling procedures for after they return.
In the modern era of office based procedures such as Closurefast RFA, Venaseal or Varithena - which are far less invasive and painful than the old techniques of vein stripping - we tell most patients they can go back to their usual activities the next day. Most patients can walk into our office, have the procedure, and walk out. If they don’t take any medications like valium, they can drive themselves home. We ask patients to take it easy the first night, but after that they are able to go back to work, exercise, and continue other daily activities.
Compression can be helpful for patients with symptoms from varicose veins. Some patients will find that compression stockings help, but not all patients benefit and some need to have procedures to help treat their veins to help them feel better.
Varicose veins do not go away on their own. They in fact tend to worsen with time.
Generally yes. Massage is great to help stimulate the nerves in the skin, veins and muscle that can help improve lymphatic flow. Also, it can help relieve sore muscles and facilitate more movement, which is great for vein health.
A healthy diet is important for vein health. Being overweight tends to make vein problems worse. Also, certain foods are known to be inflammatory for certain patients. Vein conditions involve inflammation and when foods contribute to that, varicose vein symptoms can be worse.
Walking and movement are generally helpful for vein health. This is especially true for patients with venous insufficiency (Varicose Veins). When walking, the calf veins are squeezed by the calf muscle, which helps reduce pooling of blood in the lower legs.