Although it rarely receives much attention, deep vein thrombosis (DVT) is a rather serious condition that can strike anyone at anytime. DVT can arise due to injury, after surgery or illness, or simply after a lengthy period of inactivity; Worse yet, if left untreated, DVT can become life-threatening.
Thankfully, awareness can go a long way in preventing serious complications. So, take the time to learn more about DVT in order to identify symptoms and reduce your risks!
What Does DVT Look Like?
DVT is caused when blood pools in veins, allowing a clot to form. Although this condition typically affects the veins deep in the legs, it can occur in the arms as well. The location and size of the clot determines if you will see any noticeable symptoms of the DVT.
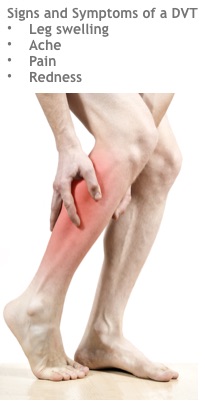
In the case of large clots, you might spot swelling in the affected area, while small clots might just make the veins appear larger than normal. In some cases, there are no visual signs at all. Since you cannot rely on visual signs alone, it is important to look a bit further before ruling out blood clots.
What are the Warning Signs of DVT?
Beyond visual indicators, there are some other warning signs of DVT to watch for, such as:
- Pain while walking or moving your arms
- Pressure in the limbs from swelling
- Excessive warmth in the affected area
- Redness of the arm or leg, especially with swelling
When an Untreated DVT Develops to Pulmonary Embolism
Not all people develop symptoms, however. Some may not even notice a problem until the clot breaks off and moves to the lungs, causing a pulmonary embolism. Then, they may start to experience chest pain, shortness of breath, and a fast heartrate.
Upon noticing any symptoms of DVT, it is important to seek immediate care to prevent a potentially deadly blood clot in the lungs. Even the slightest suspicion of blood clots should be reported to your doctor, so they can rule it out and verify you are in good health.
How to Treat Deep Vein Thrombosis
In order to find the right treatment for DVT, vein physicians assess the risk factors and causes that led to the condition. They will also look at the location of the blood clots and severity of your symptoms.
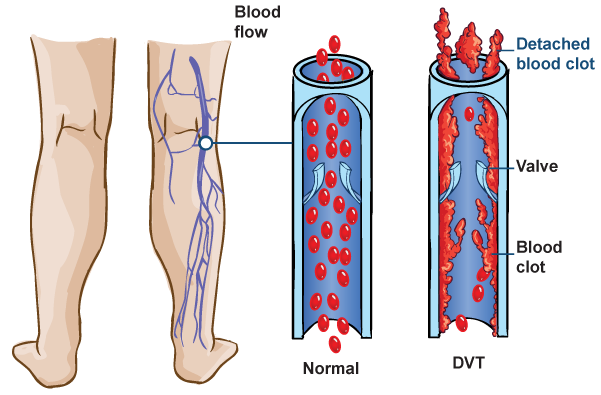
Depending on their findings, they may decide to use anticoagulation medications to thin the blood and reduce the risk of clotting. Or they may decide that catheter directed thrombolysis will better resolve the problem and protect you from life-threatening complications.
No matter what course of treatment is advised, almost all patients need to wear graded compression hose. This helps to immediately decrease the swelling and ease your pain and discomfort.
sign up for our webinar to learn more about DVT >>
Inovia Vein Specialty Center Can Help
If you notice any of the warning signs of DVT, it is important to seek care right away. Thankfully, you can count on Inovia Vein specialists to help promptly assess your symptoms and provide much-needed support. Call any of our clinics in Northwest Portland , Tigard, Happy Valley, Hillsboro or Bend, Oregon, or fill out our Online Appointment Request Form to schedule an appointment.
