We all know that symptoms from an infection with the coronavirus (COVID-19) can starts with a fever and cough. In some patients, hospitalization is required.

We are now learning that there is a significant issue with blood clotting in patients who are hospitalized for COVID-19. Blood clots, jelly-like clumps of cells and proteins, are the body’s mechanism to stop bleeding.
Normally the blood only clots when we have a cut, for example, and the blood is exposed to injured tissue as a mechanism to stop bleeding. This is normal. However, sometimes injury inside the blood vessels can lead to blood clotting inside the blood vessels. This is abnormal. Researchers have observed miniature clots in the body’s smallest vessels in COVID-19 patients.
Blood Clotting Background History
Abnormal blood clots can develop in the arteries or veins. When blood clots in arteries, it can cause a stroke or heart attack, for example. More commonly, blood clots in veins. This can be in deep or superficial veins. It can be in large or small veins. It’s called Deep vein thrombosis (DVT) when it happens in the legs (most commonly) or arms (less commonly).
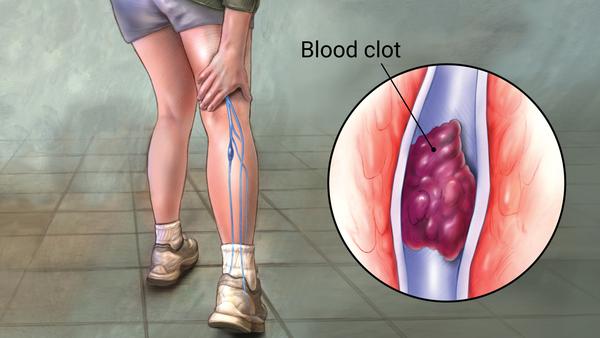
If a blood clot breaks off in a vein or artery and travels to cause a problem elsewhere, it’s called an embolism. A pulmonary embolism (PE) occurs when a blood clot breaks off and travels through the veins to the lung. They can be small, and result in cough and shortness of breath. Or they can be massive and result in sudden death. Thus DVT and PE share common risk factors and are related in that DVT is a risk for PD.
When blood clots occur, we can see traces of them in the blood with a lab test. D-dimer is a product of degradation of fibrin acting as a surrogate marker for fibrinolysis and is usually elevated in thrombotic events like DVT or PE.
COVID Patients Appear to Have Blood Clotting Problems
Initially this became suspected when studies from Asia showed markers of clotting, called D-Dimer, in the blood. Then studies from Europe revealed that venous blood clots arise in 20–30% of critically ill COVID-19 patients.
Most of these clots were initially noted in the lungs because the front line health providers were so focused on the lung problems that most sick COVID patients have. However, studies are now starting to show a large number of patients with COVID-19 have blood clots in the large veins of their legs, known as a DVT.
This suggests that not only is it possible that clots arise inside the lung veins and arteries, but also as an embolic problem from clots arising in the legs. Thus the clots can be microvascular (in the very small vessels) or macrovascular (in the big veins).
How to Diagnose Clotting Problems in COVID Patients
Sometimes these clots can be silent, so to speak, and thus they have to be suspected and looked for since the usual sign of leg swell. In this case, obtaining a venous ultrasound is a good start. This allows us to visualize all the veins in the legs (or arms) and look for clots in the bigger veins.
To look for clots inside the body (chest, abdomen or pelvis) usually requires a CT scan or MRI. The D Dimer test can provide a blood test marker for clotting in general, but it does not say where the clot is located. Also, just being sick can raise D-Dimer so the clinician has to use this information along with other clinical indicators to decide what to do with the information.
What are COVID Toes?
We are all generally aware of the most common symptoms of Coronavirus such as cough, shortness of breath, fever and loss of smell or taste. However, you may have also heard of COVID toes and how this too may be a sign to consider COVID.
This happens, generally in younger, healthier patients who develop red, purple or blue toes but otherwise do not have the typical respiratory symptoms of Coronavirus infection. There is still a lot that is not known.
Does this mean the patient has COVID? Does this go away? If so, how long? Is this a clotting issue? Is this a blood vessel spasm issue (Vasospasm)? Is this an immune response leading to a small blood vessel inflammation (Vasculitis)? Should this be treated? If so…how?
For now, this should prompt a phone call to your healthcare provider and consideration for testing and possible self-isolation until the details are sorted out. There is a lot coming out in the medical literature about this now and more will be known soon. If you have questions, start with a phone call to develop a plan for further evaluation.
Diagnose and Treat Blood Clots
If you have concerns you or a close contact may have COVID, it’s always best to start with a call to your healthcare provider. The emergency room is best reserved for emergencies (for example trouble breathing). But if you can, start by reaching out to your health provider, or as an alternative, call an urgent care facility.
If you or your healthcare provider have specific concerns about vascular clotting issues big or small, we at Inovia Vein Specialty Centers are available and can help! Simply fill out our Online Appointment Request Form or call any of our clinics in Northwest Portland , Tigard, Happy Valley, Hillsboro or Bend, Oregon.
