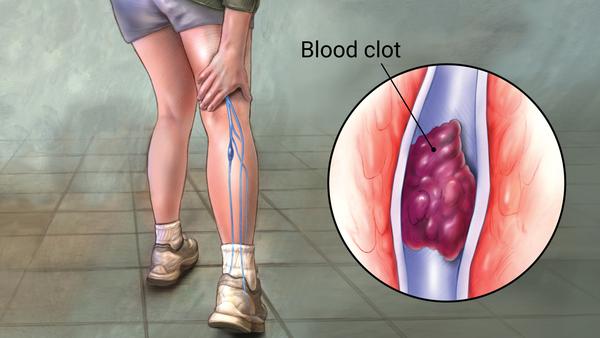
We are often asked if varicose vein treatment reduces risks of DVT. There is in fact evidence of this from patients having major orthopedic surgery.
One of the biggest risks after major orthopedic surgery, such as a knee or hip replacement, is the development of a deep venous thrombosis (DVT) or pulmonary embolism (PE). Blood clots after orthopedic surgery are associated with higher death rates, rehospitalization, costs, and bleeding within 1 year, compared to patients who do not develop blood clots after orthopedic surgery.
The strong activation of the clotting cascade that occurs during these operations places patients at increased risk for venous thromboembolism. However, patients with preexisting vein issues may be at significantly higher risks of a DVT or PE complicating their post-surgical recovery. There is growing evidence that having varicose vein treatment can reduce risk of DVT after Surgery.
Evidence of DVT Risk from Varicose Veins
It has long been known that a history of blood clots in the legs (DVT) are a risk factor for future DVT when a patient is recovering from a major orthopedic operation. However, there is now increasing evidence that just having untreated varicose veins may also be a major risk factor for a DVT when recovering from orthopedic surgery.
In a study published in the Archives of Orthopedic and Trauma Surgery (June 2015 pages 759-772) titled “Risk factors for venous thromboembolism after total hip and total knee arthroplasty: a meta-analysis” found that the presence of varicose veins was one of the top risks for developing a DVT after total hip replacement (also known as total hip arthroplasty, or THA) or total knee replacement (also known as total knee arthroplasty, or TKA).
In a similar study after total hip replacement investigators asked the question “Does previous varicose vein surgery alter deep vein thrombosis risk after lower limb arthoplasty? DVT rate in patients who had previously undergone varicose vein surgery was 0.8%, and in those with no previous VV diagnosis or surgery was 0.8%. In patients with a previous varicose vein diagnosis but no varicose vein surgery, the THA DVT rate was 3.1%. This marked increase in risk of DVT after total hip replacement was statistically significant. They concluded that untreated varicose veins are associated with an increased risk of DVT after total hip replacement. Therefore, patients with varicose veins should consider having them treated prior to undergoing orthopedic interventions.
Combined this evidence suggests that having untreated varicose veins may be a risk factor for developing a DVT after orthopedic surgery, and that varicose vein surgery can reduce the risk of DVT after orthopedic surgery.
What You Can Do to Reduce Risks of DVT After Orthopedic Surgery
In our clinic, we often see patients both before and after major orthopedic surgery and trauma. Sometimes we are seeing them to help develop strategies to “deal with their veins” after a planned orthopedic operation. These are generally patients with a history of blood clotting or DVT, or a history of varicose veins with the patient and the orthopedic team are concerned about DVT risk after surgery. We generally start by emphasizing the importance of compression stockings both before and after surgery. This helps minimize swelling which allows wounds to heal better and better mobilization of the leg. We also emphasize the importance of following the recovery protocols at the hospital and home for early frequent movement. Veins do better with movement, which minimizes pooling of blood in the legs. Most hospitals have pre existing DVT prevention protocols that include risk assessment, then DVT prevention protocols that use early mobilization.
The rates of DVT or PE complications have been shown to be around 40–60% within 7 to 14 days following orthopedic lower limb surgery without formal prevention techniques (known as thromboprophylaxis). Most hospitals have formal preventative programs to reduce the incidence of this significantly and all patients are advised to follow the local protocols to minimize the risk. Many of these operations are elective, however, and many patients have many months or years to anticipate when they might need joint replacement surgery.
You might also discuss with your surgical team if you have a history of varicose veins, varicose vein treatments, or blood clots in the veins (DVT). You can often tell by looking at your legs, where you might see:
- bulging varicose veins
- a swollen leg
- brown and red discolored skin by the ankles
- wounds around the ankle and foot that are slow to heal
These are all a signal of underlying venous disease. Given the association of varicose veins with DVT after joint surgery, and the evidence suggesting this might be reduced by treating the veins prior to the procedure, it may be prudent to seek an opinion about options for the veins prior to the major joint replacement.
Schedule a Vein Consultation
Inovia Vein Specialty Centers specialize in varicose vein care, DVT diagnostics and management, and vein health.
To learn more about varicose veins and/or DVT, simply fill out our Online Appointment Request Form or call any of our clinics in Northwest Portland , Tigard, Happy Valley, Hillsboro or Bend, Oregon.