What is a DVT?
DVT, or deep vein thrombosis, is a blood clot in the large veins of the legs (most commonly) or less commonly the arms.
The general function of the cardiovascular system (heart, lungs, and blood vessels) is to deliver oxygen and nutrients to the cells of the body. The heart pumps the blood through arteries to supply oxygen and other nutrients to the tissues throughout the body. Veins are needed to carry deoxygenated blood back to the heart and lungs.
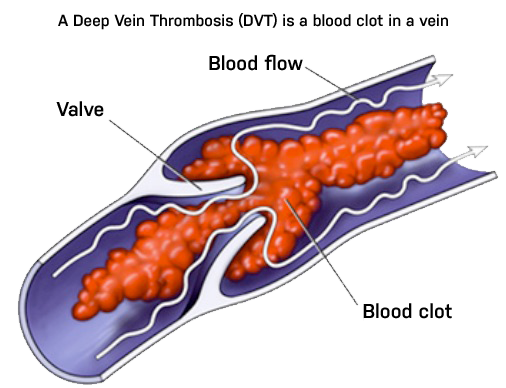
The blood from the legs must make its way against gravity back to the heart. This is done by a series of veins that have valves in them to prevent back flow of blood. As the leg muscles move, the blood is squeezed up the veins, and the valves keep the blood from flowing back down with gravity.
The veins start as a series of small parallel passages that join to form progressively larger veins, which in turn join larger and larger veins until they meet the Inferior Vena Cava, which is the largest vein in the body. The inferior vena cava is connected to and drains to the heart, where the blood is again pumped through the lungs and then is sent back out to the arteries.
The venous system to the lower part of the body can be viewed as an upside down tree, with smaller branches joining larger and larger branches until they join the inferior vena cava, which is like the tree trunk. The veins next to the skin are called superficial veins, and the veins deep to the muscle are called deep veins. The deep veins carry the majority of blood out of the leg.
A clot in the deep veins can be a serious medical condition. Another way to look it this is to think of the veins in the legs like a highway system. The deep veins are the main south to north interstate system heading to main destination (the heart). This interstate highway (deep vein) has more traffic (volume) and travels at a higher speed (pressure).
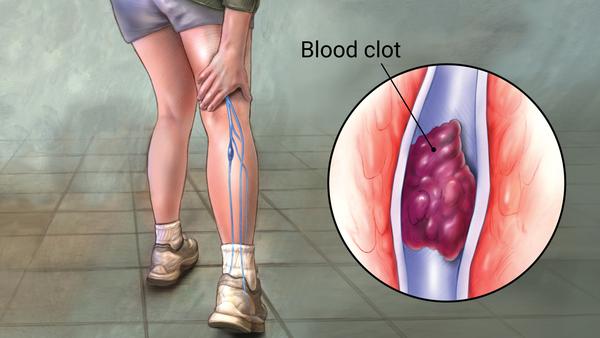
All the state highways and side roads that feed into the interstate are like the superficial veins. These have less volume and lower pressure. Eventually all roads lead back to the heart.
On a highway, what happens when there is an accident on the main interstate highway going north? Of course this can lead to a massive traffic jam. In the veins, this blockage can result in a pressure build up, and ultimately re routing of flow around the blockage. When this happens in the veins due to a clot in the deep veins, it is called a deep vein thrombosis, or DVT.
Call 1-800-834-6362 to Schedule a Consultation or Use Our
What causes DVT?
There are a number of reasons why clots can form in the deep veins. Long ago it was recognized that clots form in veins for three basic reasons which are (1) damage to the vein wall; (2) lack of blood movement (also called stasis), and; (3) a pre-disposition to form clot called hypercoagulibity.
- Damage to the vein wall
Damage to the veins can happen in a number of settings, including recent surgeries, accidents and falls or other types of trauma. Injury to the vein is a very common cause of DVT. - Lack of blood movement (stasis)
Stasis occurs when a person is immobilized for any number of reasons, including sitting in an airplane or car for long periods of time without movement, or having your leg in a cast.
- A pre-disposition to form clot called hypercoagulibity
Finally, and perhaps the least well understood, is hypercoagulability. There are certain people who for one reason or another simply have a predisposition to form blood clots. Sometimes this is due to a very subtle genetic defect where there body does not have the right balance of coagulation factors that either create or more likely, break down clot once it occurs.1 In addition to genetic factors, some patients can develop an acquired propensity to form clot. This is very common in some types of cancer, as well as after surgery or trauma.
Due to a combination of these factors, DVTs are common after certain types of surgery, especially any operation in the abdominal, pelvis, and the legs. This is especially true after orthopedic surgery, where the DVT rate can be as high as 40%.
For example, after many types of surgery, there is a variable combination of injury (from the surgery itself), stasis (from being immobilized during and after surgery) and hypercoaguabity (due to an acquired imbalance of natural coagulation factors) that make the risk of a DVT a not uncommon event after certain operations. For this reason, there are a number of efforts undertaken to try to limit DVTs after surgery.
This effort, called DVT prophylaxis, includes the use of low dose injectable blood thinners, intermittent pneumatic compression devices (leg squeezers), elastic compression stockings and early ambulation, all of which are designed to reduce the chance of a DVT at the time of surgery. Unfortunately, although the risk can be reduced, at this time it is impossible to reduce the risk of a DVT to zero.
- A pre-disposition to form clot called hypercoagulibity
Finally, and perhaps the least well understood, is hypercoagulability. There are certain people who for one reason or another simply have a predisposition to form blood clots. Sometimes this is due to a very subtle genetic defect where there body does not have the right balance of coagulation factors that either create or more likely, break down clot once it occurs.1 In addition to genetic factors, some patients can develop an acquired propensity to form clot. This is very common in some types of cancer, as well as after surgery or trauma.
Due to a combination of these factors, DVTs are common after certain types of surgery, especially any operation in the abdominal, pelvis, and the legs. This is especially true after orthopedic surgery, where the DVT rate can be as high as 40%.
For example, after many types of surgery, there is a variable combination of injury (from the surgery itself), stasis (from being immobilized during and after surgery) and hypercoaguabity (due to an acquired imbalance of natural coagulation factors) that make the risk of a DVT a not uncommon event after certain operations. For this reason, there are a number of efforts undertaken to try to limit DVTs after surgery.
This effort, called DVT prophylaxis, includes the use of low dose injectable blood thinners, intermittent pneumatic compression devices (leg squeezers), elastic compression stockings and early ambulation, all of which are designed to reduce the chance of a DVT at the time of surgery. Unfortunately, although the risk can be reduced, at this time it is impossible to reduce the risk of a DVT to zero.
Common Symptoms of DVT
DVT often occurs in the legs and may present with the following signs:
- Swelling – Usually in one leg, particularly in the calf or thigh.
- Pain or Tenderness – May feel like a cramp or soreness that worsens over time.
- Warmth – The affected area has a warmer sensation than the surrounding skin.
- Red or Discolored Skin – A reddish or bluish tint may appear on the leg.
- Visible Veins – Surface veins may become more noticeable or swollen.
Some people with DVT may experience no symptoms at all. If you suspect a blood clot, prompt medical attention is necessary.
Common Symptoms of DVT
At Inovia Vein Specialty Centers, treatment options include:
- Anticoagulant Medications – Blood thinners to prevent clot growth and reduce the risk of new clots.
- Compression Stockings – Help reduce swelling and prevent complications like post-thrombotic syndrome.
- Thrombolytic Therapy – Clot-dissolving medication quickly breaks up large clots in select cases.
- IVC Filter Placement – A filter inserted into the inferior vena cava prevents clots from reaching the lungs (for those who can’t take blood thinners).
- Lifestyle Guidance – Recommendations for movement, hydration, and long-term prevention.
How common are DVT’s?
Many people are surprised to find out how many people have a DVT each year. In the U.S., approximately 2 million patients are found to have a DVT and 600,000 patients with a DVT diagnosis will be hospitalized each year. And it is estimated that only half of people with DVT’s are actually diagnosed, meaning many people have a DVT and don’t even know it.
Unfortunately, up 200,000 people die each year due to the complication of deep vein thrombosis, mostly due to pulmonary embolism. Amazingly, many of these deaths could be prevented. DVTs are more common in individuals with risk factors.
Common risk factors for DVT include:
- surgery
- hospitalization for acute medical illness
- nursing home confinement
- trauma
- active cancer
- neurologic disease with paralysis
- varicose veins
- central venous catheters
- pacemaker (because the leads are in the deep arm veins)
Among women, there are additional significant DVT risk factors:
- oral contraceptives
- pregnancy (and immediately after pregnancy)
- hormone replacement therapy
- Also, a PE is the leading cause of maternal death associated with childbirth.
DVT has been associated with travel such as long air plane flights, a condition termed the “economy class syndrome.”